October 22, 2009 at 7:48 a.m.
National healthcare reform debate being shaped by people behind the scenes, like county public health director
Well, you could thank (or blame) Chisago County Public Health Director Jill Briggs. As a Robert Wood Johnson Executive Nurse Fellow, one of 20 in the United States, she is a participant in the health care policy program. Her assignment includes doing a lengthy project related to national health care reform. "The whole point," said Briggs, "is that we are expected to impact the discussion about reform."
Briggs opted to partner with five other public health directors to compile the costs, get financial expert analysis of the data and calculate funding gaps inherent in providing for "public health." Briggs said her research has taken into consideration everything from preparing for disasters, to tackling infectious diseases, to environmental health issues in any given community.
According to Briggs, the "cost model" she is finalizing as her fellow project is aimed at informing policymakers exactly how much it costs to address public health factors. These are not "Cadillac" expenditures, Briggs explained. She describes the study as evaluating "basic, minimum services."
Briggs traveled to Denver the first part of this month and heads to Philadelphia in November, as part of her networking requirements in the fellow program. She says there's excitement over the national healthcare issue everywhere she goes, but she also sees how complicated it is. (Travel and accommodation are paid for by the RWJ Foundation)
States all have their own methods when it comes to supporting public health. Some states approach public health as a centralized system-- with the state leading the way-- while other public health programs like Minnesota's are "decentralized," but work closely with state leaders.
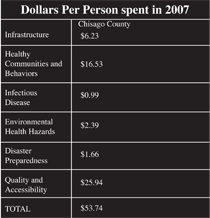
The idea behind Briggs' cost model is to allow all public health officials to speak the same language and be able to compare and contrast budgets. (See graphic for Chisago County costs.)
Public Health outcomes are next on the list, Briggs explained.
Public Health Directors need to be able to articulate exactly what a public health department expects to achieve with a certain level of expenditures.
"I am a believer in being able to stand up and tell your story, whatever it is, on how we spend tax dollars." Briggs said public health workers have been pretty good at identifying funding shortfalls and then asking for more. Directors would do a better service by being able to plug their numbers into the cost model and explain how dollars are spent and why. "All directors need to be able to speak to this," she said.
This has been an inspiring time to be involved in the foundation's health policy fellows program. About one-fifth of public health funding can come from federal programs. Usually the majority spent on public health is local dollars, with the rest made up in state tax revenues.
Briggs said once the cost model is put into use, officials can then drill a little deeper into which outcomes rely on local levy budgets, versus outside revenue.
Briggs said she expected to "...do something meaningful" when she was selected as a fellow, yet even she is a little awestruck at times with how timely her project is and its potential to influence national reform initiatives.
Health care reform is expected to be discussed further in the full House of representatives in coming weeks, as three House committees have moved versions of reform through their various reviews. In the U.S. Senate a merged version of a couple committee health care reform measures is to be debated by the full Senate.




Comments:
Commenting has been disabled for this item.